Atopic skin care revolves around three core priorities restoring your skin barrier, locking in moisture, and avoiding irritants that trigger flare-ups. If you have atopic dermatitis (the most common form of eczema), the right daily routine can dramatically reduce itching, redness, and dryness without always needing prescription medication.
A systematic review and meta-analysis published in Dermatitis estimated that atopic dermatitis affects roughly 11.1% of children and adolescents and 6.3% of adults worldwide. According to the Allergy & Asthma Network, approximately 86% of patients experience itching on a daily basis, and over 70% of adults with the condition report a negative impact on their mental health. These numbers make one thing clear: a reliable, gentle skin care strategy is not optional it is essential.
This guide walks you through every step of building an effective atopic skin care routine, from choosing the right cleanser to identifying hidden triggers that sabotage your progress.
Table of Contents

What Is Atopic Skin and Why Does It Need Special Care?
Atopic skin is skin that is genetically predisposed to dryness, inflammation, and an impaired protective barrier. It is the underlying condition behind atopic dermatitis a chronic, relapsing form of eczema characterized by intense itching, redness, and flaking.
Unlike ordinary dry skin that responds well to any standard lotion, atopic skin has a fundamentally weakened outer layer. This means moisture escapes more rapidly, and irritants, allergens, and bacteria penetrate more easily. Research published in the British Journal of Dermatology estimated that over 204 million people globally live with atopic dermatitis, making it the single largest contributor to the worldwide burden of skin disease.
Because the skin barrier itself is compromised, atopic skin demands products and routines specifically designed to repair, protect, and hydrate not just at surface level, but at the deeper structural layer where ceramides and lipids maintain skin integrity.
The Skin Barrier Problem: Why Atopic Skin Loses Moisture
In atopic dermatitis, the skin barrier is structurally deficient it lacks adequate ceramides, natural oils, and moisture-retention factors. This deficiency is often linked to genetic variations in the filaggrin protein, which plays a central role in holding the outer skin layer together.
When this barrier breaks down, two things happen simultaneously:
- Water escapes outward through a process called transepidermal water loss (TEWL), leaving skin chronically dehydrated.
- Irritants and allergens move inward, provoking the immune system into an inflammatory response that causes redness, swelling, and relentless itching.
This is why simple moisturizing alone is often not enough. Effective atopic skin care must actively rebuild the barrier using targeted ingredients not just coat the surface temporarily.
How to Build a Daily Atopic Skin Care Routine
A proper eczema skin care routine follows three essential steps: gentle cleansing, immediate moisturizing, and daily sun protection. Keeping it simple reduces the risk of irritation while covering every base your skin needs.
Step 1: Gentle Cleansing
Harsh soaps, sulfates, and foaming cleansers strip the already fragile oils from atopic skin. The American Academy of Dermatology (AAD) advises bathing in warm never hot water for no longer than 5 to 10 minutes. Use a mild, fragrance-free liquid cleanser rather than traditional bar soap.
Key cleansing rules for atopic skin:
- Choose soap-free, pH-balanced formulas that preserve the skin’s acid mantle.
- Avoid scrubbing or using rough washcloths pat gently instead.
- Limit baths and showers to once daily to prevent over-stripping natural lipids.
Step 2: Moisturize Immediately After Washing
This is the single most important step in any atopic skin care routine. Harvard Health describes moisturizing as the first line of defense against eczema flare-ups, recommending thick creams and ointments over thin lotions.
Apply moisturizer within three minutes of bathing while your skin is still slightly damp. This traps water against the surface and allows emollients to seal it in. The National Eczema Association recommends using hypoallergenic, petroleum-based ointments for maximum moisture retention, especially during active flares.
For best results, moisturize at least twice daily once after your morning wash and once before bed.
Step 3: Apply Sunscreen Daily
UV exposure weakens an already compromised skin barrier and can trigger inflammation in eczema-prone skin. However, chemical sunscreen ingredients like oxybenzone and octinoxate are known irritants for sensitive skin.
Choose a mineral-based sunscreen with these features:
- Active ingredients: Zinc oxide or titanium dioxide only.
- SPF level: Broad-spectrum SPF 30 or higher.
- Formula: Fragrance-free, hypoallergenic, and designed for sensitive skin.
Mineral sunscreens sit on top of the skin and physically block UV rays rather than being absorbed, which makes them far less likely to cause stinging or flare-ups on atopic skin.
Here is the second half of the atopic skin care article, continuing exactly where the first half ended:
Best Ingredients for Atopic Dermatitis Skin Care
The most effective atopic skin care products contain ingredients that actively repair the skin barrier, attract moisture, and calm inflammation. Not all moisturizers are created equal what works for normal dry skin can actually irritate eczema-prone skin further.
Here are the gold-standard ingredients to look for, as recommended by the National Eczema Association:
| Ingredient | What It Does | Best For |
| Ceramides | Rebuild the lipid barrier between skin cells | All atopic skin types |
| Colloidal oatmeal | Reduces itch and soothes inflamed skin | Active flare-ups |
| Petroleum jelly (petrolatum) | Seals moisture and blocks irritant entry | Severe dryness, nighttime use |
| Glycerin | Draws water into the outer skin layer | Daily lightweight hydration |
| Hyaluronic acid | Capable of retaining water up to 1,000 times its own weight. | Boosting hydration under thicker creams |
| Niacinamide (Vitamin B3) | Supports immune-mediated skin repair | Redness and uneven texture |
When choosing products, prioritize thick creams and ointments over lightweight lotions. Harvard Health specifically recommends brands such as CeraVe, Vanicream, and Eucerin, as well as plain petroleum jelly, for their proven ability to restore and protect the atopic skin barrier.
Ingredients to Avoid With Eczema-Prone Skin
Certain common skincare ingredients can worsen atopic dermatitis by stripping natural oils, provoking immune reactions, or disrupting the skin’s pH balance. Knowing what to avoid is just as critical as knowing what to use.
Steer clear of these in any product that touches your skin:
- Fragrance (including “natural” fragrance): According to the National Eczema Association, fragrances are responsible for 30-45% of allergic reactions in cosmetic products. Even products labeled “unscented” may contain hidden masking fragrances.
- Sodium lauryl sulfate (SLS): A harsh foaming agent found in many cleansers and shampoos that strips the lipid barrier aggressively.
- Alcohol (denatured or isopropyl): Evaporates rapidly and pulls moisture out of already dehydrated skin.
- Retinoids: While popular in anti-aging routines, retinoids accelerate cell turnover in a way that can aggravate irritation and dryness on atopic skin.
- Dyes and artificial colorants: Offer no skin benefit and carry unnecessary sensitization risk.
A practical tip: always read the full ingredient list, not just the front label. The AAD recommends patch-testing any new product by applying a small amount to your inner arm daily for 7 to 10 days before using it on larger areas.
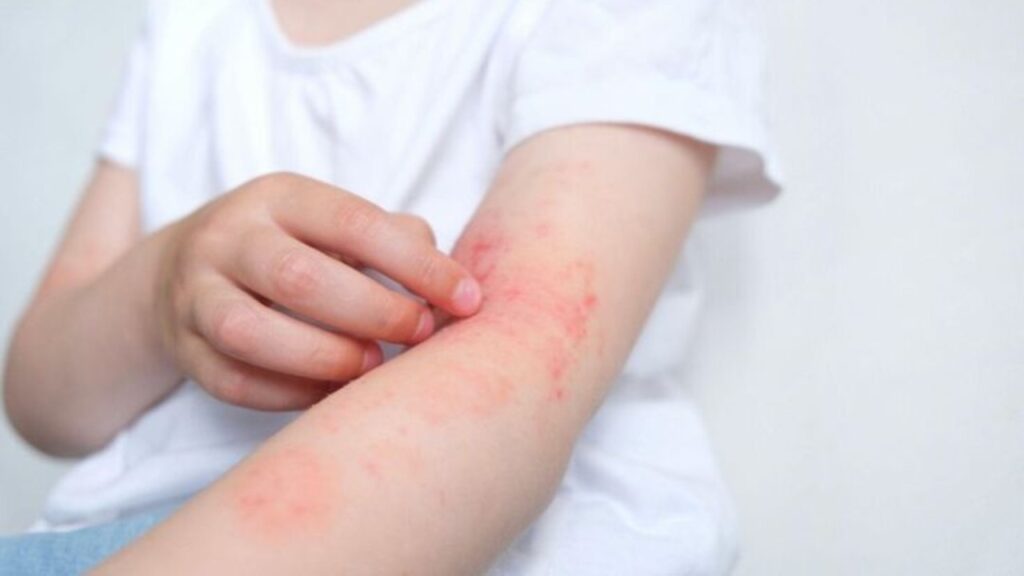
Common Triggers That Worsen Atopic Dermatitis
Atopic skin reacts not only to what you put on it, but also to environmental, dietary, and emotional triggers. A research review published in PMC (PubMed Central) identified several major categories of triggers that aggravate eczema symptoms.
The most frequently reported triggers include:
- Harsh soaps and detergents including laundry products that leave irritant residue on clothing and bedding.
- Wool and synthetic fabrics cotton is best tolerated by most atopic skin patients.
- House dust mites a leading indoor allergen that worsens eczema in sensitized individuals.
- Temperature extremes both hot, humid weather and cold, dry air can provoke flare-ups.
- Emotional stress psychological stress activates inflammatory pathways that directly impact skin.
- Sweat while exercise is healthy, trapped perspiration irritates inflamed skin and triggers itching.
Keeping a simple written log of your flare-ups alongside daily activities, foods, and weather changes can help you identify your personal triggers over time. Pattern recognition is one of the most powerful tools in long-term eczema management.
When to See a Dermatologist
If your atopic skin care routine is not controlling flare-ups, or if your skin becomes cracked, weepy, or infected, it is time to consult a board-certified dermatologist. Self-care has its limits, and prescription-level treatment may be necessary to break the cycle.
You should seek professional care if:
- Over-the-counter moisturizers and gentle routines no longer provide relief.
- Itching disrupts your sleep on a regular basis.
- You notice signs of skin infection oozing, crusting, warmth, or yellow discharge.
- Eczema patches spread to new areas or become significantly worse over a short period.
Dermatologists can prescribe topical corticosteroids, calcineurin inhibitors, or newer biologic therapies depending on severity. According to a 2024 study published in the Journal of the European Academy of Dermatology, the treatment landscape for atopic dermatitis has expanded significantly in recent years, with multiple new targeted therapies now available for moderate-to-severe cases.
Conclusion: Consistency Is the Key to Managing Atopic Skin
Effective atopic skin care is not about finding one miracle product. It is about building a consistent, gentle routine that protects your barrier, locks in hydration, and avoids the ingredients and triggers that set off inflammation. Cleanse with care, moisturize immediately and often, shield your skin from UV damage with mineral sunscreen, and pay close attention to what your skin reacts to.
The statistics make the stakes clear hundreds of millions of people deal with this condition daily, and the majority report significant effects on both their physical comfort and mental health. But with the right approach, flare-ups become less frequent, less intense, and far more manageable.
Start with one small change today swap out a fragranced product for a fragrance-free alternative, or commit to moisturizing within three minutes of every shower. Share this guide with someone who struggles with eczema, and leave a comment below with the tip that helped you most.
Frequently Asked Questions
What is the best daily routine for atopic skin care? The most effective daily routine for atopic skin involves three steps: cleansing with a gentle, fragrance-free wash in lukewarm water, applying a ceramide-rich moisturizer to damp skin immediately after, and finishing with a mineral-based SPF 30+ sunscreen. Repeating the moisturizing step before bed provides overnight barrier repair.
Can atopic dermatitis be cured with skin care alone? Atopic dermatitis is a chronic condition with no permanent cure, but a consistent skin care routine can significantly reduce both the frequency and severity of flare-ups. In mild cases, proper moisturizing and trigger avoidance may be enough to keep symptoms fully under control without prescription treatment.
What type of moisturizer is best for eczema-prone skin? Thick creams and ointments outperform lightweight lotions for atopic skin because they create a stronger seal against moisture loss. Look for formulas containing ceramides, petrolatum, or colloidal oatmeal, and make sure the product is labeled fragrance-free and hypoallergenic.
Is fragrance-free the same as unscented? No and this distinction matters greatly for eczema sufferers. “Fragrance-free” means no fragrance chemicals have been added, while “unscented” products may still contain masking fragrances that can trigger allergic reactions. Always choose products explicitly labeled “fragrance-free.”
How often should I moisturize if I have atopic dermatitis? Dermatologists generally recommend moisturizing at least twice a day once in the morning and once at night with additional applications after hand washing, bathing, or any time the skin feels tight and dry. When symptoms are at their peak, applying it more often may be required
When should I see a doctor about my eczema? Seek professional help if your eczema worsens despite a consistent skin care routine, if sleep is regularly disrupted by itching, or if you notice signs of infection such as oozing, crusting, or unusual warmth around affected patches. A dermatologist can offer prescription therapies tailored to your severity level.

